 The Weber and the Rinne test ( / ˈ r ɪ n ə/ RIN-ə) are typically performed together with the results of each combined to determine the location and nature of any hearing losses detected. The Weber test has had its value as a screening test questioned in the literature. The outer ear consisting of the pinna, ear canal, and ear drum or tympanic membrane transmits sounds to the middle ear but does not contribute to the conduction or sensorineural hearing ability save for hearing transmissions limited by cerumen impaction (wax collection in the ear canal). Sensorineural hearing ability is mediated by the inner ear composed of the cochlea with its internal basilar membrane and attached cochlear nerve (cranial nerve VIII). Conductive hearing ability is mediated by the middle ear composed of the ossicles: the malleus, the incus, and the stapes. The test is named after Ernst Heinrich Weber (1795–1878). It can detect unilateral (one-sided) conductive hearing loss (middle ear hearing loss) and unilateral sensorineural hearing loss (inner ear hearing loss). The Weber test is a screening test for hearing performed with a tuning fork. Large ear canal volume suggests patent pressure equalization tube or perforated eardrum.The Weber test is administered by holding a vibrating tuning fork on top of the patient's head. Small ear canal volume suggests ear canal occlusion. The Jerger system is commonly used to classify tympanometric results: For example, acoustic trauma (noise-induced loss) often results in a loss centered around 4 kHz with recovery at higher frequency (i.e., a 4-kHz notch) presbycusis often involves symmetric downsloping loss, worse at higher frequency a fluctuating low-frequency loss is often seen with Ménière′s disease. Patterns of SNHL may be suggestive of certain etiologies, taken together with clinical history and exam. Basic Otorhinolaryngology: A Step-by-Step Learning Guide. (c) The type C tympanogram has a peak in the negative pressure region below −100 daPa, consistent with impaired middle ear ventilation. A type B tympanogram with large volume is seen with the perforation. This indicates immobility of the tympanic membrane, which may be due to fluid in the middle ear or tympanic atelectasis. (b) The type B tympanogram is flat or has a very low, rounded peak. 
(a) The normal tympanogram has a prominent, sharp peak between +100 and −100 daPa. 3.8 Normal and abnormal tympanogram patterns. A poor word-recognition score, especially out of proportion to pure tone thresholds, suggests possible retrocochlear pathology, such as an acoustic tumor. In a sensorineural loss, bone conduction thresholds typically equal air conduction, and the loss may be due to dysfunction at the level of the cochlea, CN VIII, or central pathways. The loss may be due to dysfunction involving the external canal, tympanic membrane, or ossicular chain or to middle ear fluid. In a conductive loss, there is an air–bone gap on the audiogram, with better bone conduction thresholds, with appropriate masking. Otologic disease may be categorized as conductive hearing loss, sensorineural loss (SNHL), or mixed hearing loss. Red flags should prompt referral to an otolaryngologist (discussed below). 3.8) may suggest various forms of otologic disease. Results of the audiogram and tympanogram ( Fig. 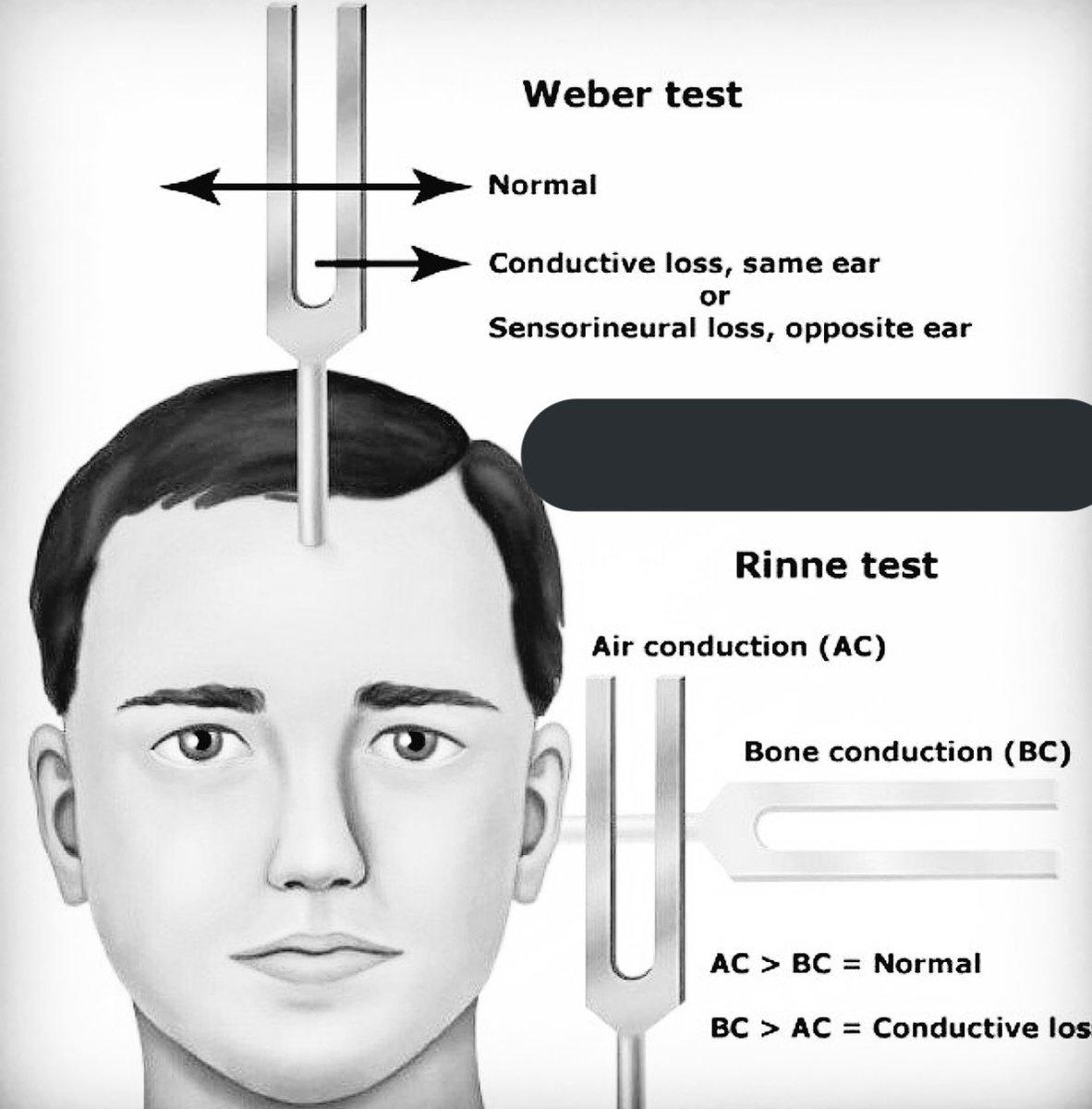
(Used with permission from Probst R, Grevers G, Iro H. (d) Audiogram showing mixed hearing loss. 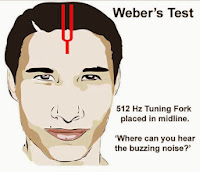
(c) Audiogram showing sensorineural hearing loss. (b) Audiogram showing conductive hearing loss. It is necessary to employ masking (a static type of noise) in certain situations to prevent the nontest ear from detecting the test signal. An audiogram is a graph with frequency (in Hz) plotted on the x axis and intensity (in dB) plotted on the y axis. Results of audiometric testing are typically plotted on an audiogram ( Fig. 
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
